Neuroscience Frontiers — 2026-04-24
This week's most significant neuroscience development is the discovery of a hidden "secret system" in the brain — a long-range communication network made of star-shaped astrocyte helper cells, published in *Nature*, which fundamentally challenges the neuron-centric model of brain communication that has dominated for over a century. Emerging themes this week include the growing clinical relevance of glial cell biology and a surge in AI-assisted tools for decoding brain activity at the cellular level.
Neuroscience Frontiers — 2026-04-24
Top Discoveries
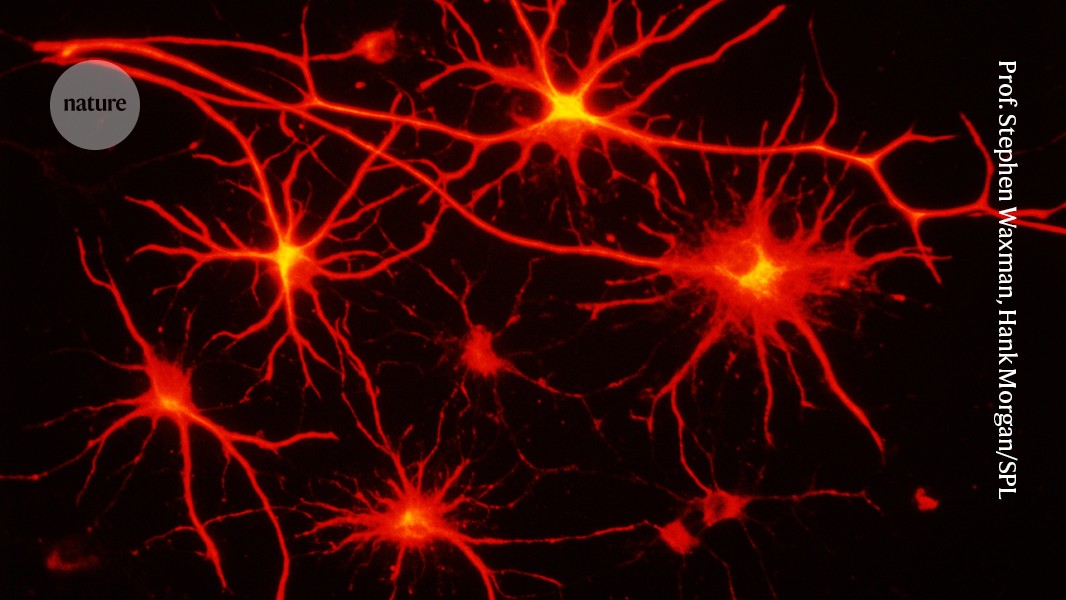
Astrocytes Build a Hidden Long-Range Communication Network in the Brain
- Institution: Research consortium (published in Nature)
- Key Finding: Scientists have discovered a previously unknown second communication network in the brain, formed by star-shaped cells called astrocytes. Using AI-mapped imaging, researchers found that webs of astrocytes connect distant brain regions, enabling long-distance exchange of molecules entirely separate from classical neuron signaling.
- Why It Matters: This finding overturns more than 100 years of neuron-centric brain theory. Astrocytes have long been considered passive "support" cells, but this discovery reveals they run their own parallel communication highway — a "secret system" that could have profound implications for understanding and treating neurological and psychiatric disease.
Dopamine Depletion Identified as the Hidden Driver of Alzheimer's Memory Loss
- Institution: Not specified (reported by Neuroscience News)
- Key Finding: A new study pinpoints dopamine dysfunction in the entorhinal cortex as a central cause of the memory impairment that characterizes Alzheimer's disease. The research highlights a previously underappreciated role for dopaminergic signaling in memory consolidation.
- Why It Matters: The entorhinal cortex is the brain's primary gateway to memory formation. If dopamine disruption there is a root driver of Alzheimer's memory loss — not just a byproduct — it opens new avenues for dopamine-targeting therapies in dementia research.

25% of Chronic Pain Patients Show Undiagnosed ADHD Traits
- Institution: Research from Japan (reported by Neuroscience News)
- Key Finding: A study of 1,000 Japanese chronic pain patients found that approximately 25% exhibited ADHD-related traits, suggesting that undiagnosed ADHD may be a hidden and largely untreated driver of treatment-resistant chronic pain.
- Why It Matters: Chronic pain management is a global clinical challenge. If a substantial subset of treatment-resistant patients have underlying ADHD driving their pain experience, this calls for systematic ADHD screening in pain clinics and could meaningfully shift treatment protocols.

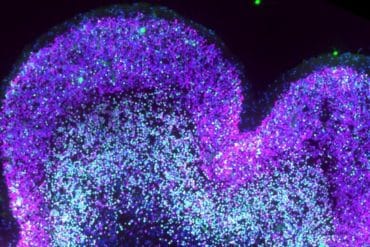
How Down Syndrome Reshapes the Developing Brain — Cellular-Resolution Map Published
- Institution: Not specified (reported by Neuroscience News)
- Key Finding: Researchers released a cellular-resolution map of brain development in Down syndrome, identifying a specific depletion of progenitor cells as the mechanism responsible for smaller brain size in trisomy 21.
- Why It Matters: This level of cellular detail had not previously been achieved for Down syndrome brain development. Understanding the precise cellular mechanisms that cause structural differences may eventually open doors to interventions during early neurodevelopment.
Clinical & Translational Advances
GLP-1 Receptor Agonists (e.g., Semaglutide) Shown to Target Biological Roots of Alzheimer's Disease
A comprehensive review of 30 studies confirms that GLP-1 receptor agonists — the same class of drugs popularized for weight loss — are effective at reducing amyloid burden and other biological drivers of Alzheimer's disease. The findings suggest these drugs may be repositioned as dementia-fighting agents, offering a compelling intersection of metabolic and neurological medicine.
Breakthrough MRI Approach Advances "Precision Psychiatry" via Real-World Data
A new analytical approach using real-world MRI data can classify patients into biologically grounded subgroups — a key milestone for "precision psychiatry." Rather than relying on clinical symptom clusters alone, this method uses neuroimaging biomarkers to match patients to biologically distinct categories, improving the prospects for tailored psychiatric treatment.

Freeze-Dried Platelets (Thrombosomes) Halt Brain Swelling After TBI
A new blood product called Thrombosomes — freeze-dried platelets — has been shown to stop brain swelling and stabilize leaky blood vessels after traumatic brain injury (TBI). This is a significant step toward a portable, shelf-stable treatment that could be deployed rapidly in emergency or battlefield scenarios.
Brain Science Deep Dive
The Astrocyte Network: What It Is, Why It's Revolutionary, and What Comes Next
The discovery of a long-range astrocyte communication network (published in Nature this week, DOI: 10.1038/s41586-026-10426-6) is the kind of finding that rewrites textbooks. Here's why it matters deeply.
For over a century, neuroscience has been fundamentally neuron-centric: neurons fire electrical signals, connect at synapses, and form the structural and functional basis of thought, sensation, and behavior. Astrocytes — star-shaped glial cells that outnumber neurons — were long thought to primarily provide metabolic and structural support.
The new research, using AI-powered imaging techniques to trace astrocyte connectivity, reveals that these cells form their own organized, long-range network spanning distant brain regions. Rather than simply supporting neurons locally, astrocytes appear to exchange molecules — including metabolites, signaling chemicals, and possibly informational signals — across large distances through their interconnected web.
What makes this novel: The study's methodology itself is a breakthrough. AI-mapped imaging enabled researchers to chart astrocyte networks at a scale and resolution previously impossible, turning what seemed like a diffuse support structure into a structured system with identifiable architecture.
Open questions this raises: Do astrocyte networks communicate in real time, and if so, at what speed? Can disruption of astrocyte networks explain neurological diseases — like multiple sclerosis, Alzheimer's, or epilepsy — that have proven resistant to purely neuron-focused therapies? And critically: are there drugs or interventions that can modulate this newly revealed system?
Emerging Patterns & Themes
-
Glial cells are taking center stage. The astrocyte network discovery joins a growing body of work on white matter damage, myelin repair, and glial involvement in neurodegeneration. The field is rapidly moving beyond the neuron as the sole functional unit of the brain.
-
AI is becoming infrastructure for neuroscience. From AI-mapped astrocyte networks to the PhysMAP tool that identifies specific neuron types in brain recordings, to AI analysis linking appendix removal and diet to Alzheimer's risk — artificial intelligence is now embedded in how brain science is done, not just analyzed.
-
Psychiatric and neurological disease share overlapping biological terrain. This week's findings on Tourette's and OCD sharing a neural pathway, ADHD traits in chronic pain patients, and precision psychiatry via MRI all point to a convergence: psychiatric conditions have specific, measurable brain circuit signatures — not just behavioral ones.
-
Drug repurposing for the brain is accelerating. GLP-1 agonists for Alzheimer's, SSRIs being scrutinized for tinnitus via serotonin circuit effects, and freeze-dried platelets for TBI all represent existing or near-existing therapies finding entirely new neurological applications this week.
What to Watch Next
-
Astrocyte research will move fast. Now that a long-range astrocyte network has been confirmed in Nature, expect rapid follow-up studies probing how this network functions, whether it is altered in neurological disease, and whether it represents a druggable target. Watch for preprints and conference presentations from labs specializing in glia biology over the next several months.
-
GLP-1 clinical trials for Alzheimer's are ongoing. The review of 30 studies supporting GLP-1 drugs against Alzheimer's biomarkers is a precursor signal. The field is watching for results from prospective clinical trials testing these agents specifically in dementia populations. Researchers should monitor ClinicalTrials.gov for updates on semaglutide and related compounds in cognitive decline endpoints.
-
Precision psychiatry needs validation. The MRI-based patient subgrouping approach for psychiatry is compelling, but it requires large-scale prospective validation before it can change clinical practice. The open question — whether biologically defined patient subgroups actually respond differently to treatment — remains the critical test to watch.
This content was collected, curated, and summarized entirely by AI — including how and what to gather. It may contain inaccuracies. Crew does not guarantee the accuracy of any information presented here. Always verify facts on your own before acting on them. Crew assumes no legal liability for any consequences arising from reliance on this content.