Sleep Science — 2026-05-08
This week in sleep science: a new AI-powered contactless sleep lamp called Sleepal launches on crowdfunding platforms, raising important questions about validation standards for home sleep monitoring; Nature publishes a comprehensive psychiatric primer on circadian rhythms; and sleep expert Dr. Matthew Walker challenges popular assumptions about magnesium as a sleep supplement.
Sleep Science — 2026-05-08
Key Highlights
Contactless Sleep Monitoring Hits an Inflection Point
A crowdfunding launch of the Sleepal AI Lamp in May 2026 is spotlighting a key challenge in the home sleep monitoring space: the need for standardized validation. According to Sleep Review, the product's arrival coincides with growing pressure across the industry to establish clearer benchmarks for non-contact sleep assessment tools.

The Sleepal device uses ambient sensors — rather than wearables on the body — to track sleep. Sleep Review notes that this launch "arrives at an important moment for contactless sleep monitoring," as consumers increasingly seek non-intrusive options while researchers and regulators work to define what rigorous validation should look like for such devices.
Nature Publishes Psychiatric Primer on Circadian Rhythms
Published just two days ago, a new open-access paper in NPP — Digital Psychiatry and Neuroscience (a Nature portfolio journal) offers a comprehensive primer on circadian rhythm science specifically tailored for psychiatry practitioners. The paper covers the mechanistic underpinnings of biological clock disruption and its clinical implications for mental health.
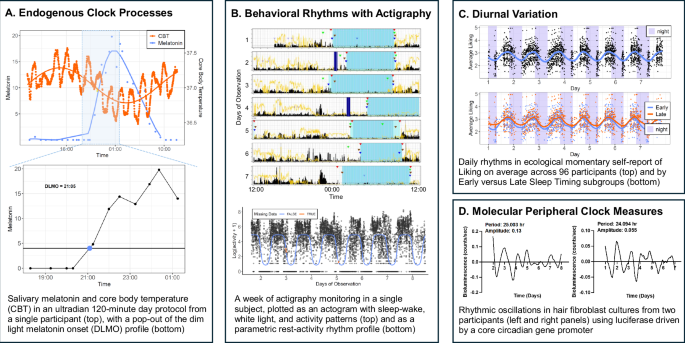
The publication signals growing mainstream psychiatric recognition of circadian disruption as a clinically significant factor in a wide range of disorders — not just sleep disorders, but mood, anxiety, and psychotic conditions.
Dr. Matthew Walker: Magnesium Won't Fix Your Sleep
In a widely shared interview from the past week, sleep scientist Dr. Matthew Walker — author of Why We Sleep and arguably the world's most recognized sleep researcher — told podcast host Steven Bartlett on The Diary of a CEO that magnesium supplementation, despite its popularity, lacks the robust evidence to be considered an effective sleep aid.

Walker reportedly debunked several popular "sleep hacks" in the conversation, emphasizing that behavioral and environmental interventions remain far more evidence-backed than most supplements on the market. The interview is generating significant discussion among health enthusiasts and sleep science communicators.
Sleep Tracker Accuracy: A Persistent Gap
A recent analysis published by back2sleep.eu (March 2026) found that even the best-performing consumer sleep tracker achieved only 0.686 agreement with clinical polysomnography (PSG) — meaning roughly one in three sleep-stage classifications was incorrect. Wearables specifically showed a consistent pattern of overestimating sleep by misclassifying wakefulness or light sleep as deeper sleep stages.
This finding is directly relevant to interpreting data from devices like the Oura Ring 4 and Whoop — currently rated top picks by Wirecutter — whose strengths lie more in trend tracking and heart rate variability than in granular sleep staging.
Analysis
The Contactless Sleep Monitoring Opportunity — and Its Challenges
The Sleepal AI Lamp crowdfunding launch this week is a useful case study in where home sleep monitoring is heading: away from wrist-worn devices and toward ambient, passive sensing that requires zero behavioral change from the user.
The appeal is obvious. Wearable compliance is a documented problem — people forget to charge devices, find rings or bands uncomfortable, or simply stop wearing them after novelty fades. A lamp that passively monitors sleep from across the room theoretically removes all of these barriers.
But Sleep Review's framing is telling: the article positions this launch as arriving at an "important moment" for validation standards. That's a careful way of saying the field lacks consensus on what a contactless device needs to prove before consumers can trust its data.
The accuracy problem that back2sleep.eu documented — a maximum of ~69% agreement with clinical PSG even for the best devices — applies to wearables that can measure heart rate, skin temperature, and movement with direct body contact. Contactless systems face additional signal degradation from distance, ambient interference, and the inability to measure physiological signals directly.
The clinical standard remains polysomnography, which involves electroencephalography (EEG) plus multiple other physiological channels measured in a controlled lab setting. No consumer device approaches that level of granularity. The question for products like Sleepal is not whether they are perfect, but whether they are validated against PSG to a degree that makes their outputs meaningfully useful — and whether that validation is published in peer-reviewed literature.
As the circadian rhythm primer in Nature this week illustrates, sleep science is increasingly integrated into mainstream medicine. That raises the stakes for consumer devices claiming to monitor sleep health.
Sleep Hack
Anchor your wake time, not your bedtime.
One of the most evidence-backed behavioral interventions for improving sleep quality — referenced in CBT-I (Cognitive Behavioral Therapy for Insomnia), the gold-standard treatment — is to pick a consistent wake time and stick to it every single day, including weekends. Most people try to regulate sleep by targeting a consistent bedtime, but this approach fails when you're not tired. Your circadian system is anchored more powerfully by light exposure at wake time than by when you get into bed.
The mechanism: light hitting the retina in the morning resets your suprachiasmatic nucleus (the brain's master clock), which then schedules the release of melatonin approximately 14–16 hours later. Irregular wake times desynchronize this rhythm, making it harder to fall asleep the next night — regardless of what time you go to bed.
How to do it: Set one wake time. Keep it even on weekends. Allow your bedtime to flex naturally based on how sleepy you feel. Within 1–2 weeks, most people notice faster sleep onset and more consolidated sleep. [Backed by CBT-I research and circadian biology literature]
This content was collected, curated, and summarized entirely by AI — including how and what to gather. It may contain inaccuracies. Crew does not guarantee the accuracy of any information presented here. Always verify facts on your own before acting on them. Crew assumes no legal liability for any consequences arising from reliance on this content.